Clinical Evaluation on Depth of the Burns Wound
作者:Rong Xiang Xu 出版社:KARGER 发行日期:In 2004Since burns wounds are conventionally treated with dry-exposed therapy or bandaging method, the resultant obscuring of the wound by scar or dressing prevents inspection of the wound the next day. People can only see the crust and the dressings, thus it becomes very difficult to estimate wound depth accurately. Though some instruments have been invented for diagnosis of burn depth, their accuracy typically proves to be less than visual estimates by experienced doctors. One advantage of burns regenerative medicine and therapy (MEBT/MEBO) is that burns wounds can be inspected in the whole treatment process by the naked eye. This allows doctors to accurately observe the changes in the wound over time, thus allowing for simple determination of wound depth. At this point, thanks to accurate observation of the pathological changes in the burn area, the clinical characteristics of burns wounds and the clinical diagnosis of burn depth can be summarized as follows.
1. First-degree burn
Diagnosis of first-degree burns is the same as the conventional surgical standard. The burns wound is erythematous in appearance, has no blister, may be painful and have slight swellings. These wounds typically heal spontaneously by 3 days postburn with varying degrees of epithelial exfoliation. The injured area should not be included when estimating the total extent of the burn since, pathologically speaking, skin was only thermally irritated and not burned, as there was no structure injury to epidermal basal layer and no formation of zone of stasis. MEBO can accelerate the recovery of first-degree burn with resolution of erythematous skin within 24 h and immediate cessation of pain. The injured epithelia in the superficial layer of epidermis can be exfoliated and removed together with the MEBO and no systemic reaction occurs.
2. Second-degree burn
Worldwide, the incidence of second-degree burns is clinically the highest. The pathological changes of second-degree burn are very complicated and, until now, quite difficult to manage. Second-degree burn is often painful and sensitive to pin-pick. The microcirculation in the injured tissue is damaged. Congestion and exudation occur, and the zone of stasis may exist in dermis. When progressive necrosis of the dermal tissue occurs due to microthrombosis formation, this worsen the clinical picture. Second-degree burns destroy the skin barrier and result in a serial systemic reaction and infection. Without application of BRT, as epithelial tissue is seriously injured, the wounds healed with disfiguring and painful scar formation dooming the patient to a lifetime of suffering.
The diagnosis of second-degree burns is not difficult. However, with conventional burns treatments, it is difficult to differentiate between superficial and deep second-degree burns because the wounds can not be inspected directly and clearly. Therefore, the diagnosis is based only on doctor’s conception of the process and not on direct experience. However, when burn regenerative medicime and therapy (MEBT) is applied, there is direct and adequate evidence for establishing the correct diagnosis.
(1). Superficial II-degree burn
• Scald wound: Within 2 h post-scald, obvious color change occurs in the dermis and blisters of different size appear. After blister exfoliation, the skin tissue looks moist, slightly red with exudation and has good elasticity. Fine hair stands straight and is sensitive to pain when pulled out. The wound is smooth. Two hours later, wound exudate increases with bright red color, and wound swelling (especially wounds in the face). 48 h later, swelling subsides and exudate decreases gradually. Four days later, epidermis of the wound thickens and the wound heals in about 6 days.
• Burns wound: The wounds may appear different appearances according to different causes, e.g. epidermal layer of the wound burned by a gas fire flame has a dark color. Compared with scald wound, wound surface caused by flame is drier and after removal of the blisters, the wound looks dark red, because flame results in serious dehydration. Pathological changes in burns wounds caused by flame are the same as in scald wounds.
(2). Deep second-degree burns
Deep second-degree burns may be further differentiated into two subtypes: 1) superficial subtype of deep second-degree burn with thermal injuries reaching the dermal papilla layer; 2) deep subtype of deep second-degree burn with injuries reaching dermal reticular layer. The key points to distinguishing the deep second-degree burn from superficial second-degree burn at the early stage are that in the former, the necrotic layer and the zone of stasis do exist in the dermis of the wound, while in the latter, (superficial second-degree burn), there is no formation of either the necrotic layer or the zone of stasis. Therefore, in the treating procedure, superficial second-degree burns wounds do not have liquefied products of necrotic tissue, while deep second-degree burns wounds produce copious amounts of liquefied products from necrotic tissue before the wound healing.
• The superficial subtype of deep second-degree burns wounds. The appearance of this type of wound is similar to superficial second-degree burns wounds. Scald wounds have blisters of different size and after blister exfoliation, the dermal tissue looks light red or pale with much exudate. The wound has good elasticity. 24 h later, numerous red pin-spots appear in the pale wound while the superficial layer of the dermis becomes semi-transparent, sensitive to pain, and gives a positive reaction when the hair is pulled out. After the exudation stage, the wound looks red, superficial layer of the dermis begins to liquefy, the base of the wound is in a position lower than skin surface. In about 10 days, liquefaction products decrease, the wound grows up to the skin surface. Healing occurs within about 15 days without scar formation. Hyperpigmentation may appear temporarily. After 1 month, the skin color recovers to normal. The burns wounds appear dark or brown in the dermis at the early stage and blisters of different size may exist. After removal of the blisters, the dermis looks red alternating with white. Exudate occurs but fine hair disappears. The wound is sensitive to pain, gives positive reaction to needle stab test. After exudation stage, the wound looks red much as the scald wound does.
• The deep subtype of deep second-degree burns wounds. At the early stage postburn, no blister appears, or small blisters may appear after a while. Scald wounds with no blister have epidermis separated and adhered to the dermis. Flame burns wound is dry with black carbonized substances on the epidermis. The wound is obtuse to pain. Some patients even have no pain sensation. If treated inappropriately, loss of pain sensation will continue, which is an unnecessary and unfortunate consequence. After removal of dead epidermis, the wound looks pale and leathery. In the deep region, dark red spots may be seen. The wound surface is dry with less exudate. After the exudation stage, the necrotic layer begins to liquefy. At this point, the wound base is obviously recessed relative to the skin surface. The wound heals to the skin surface in about 25 - 28 days. Generally, scar formation is not obvious. Often the final skin color is not uniform as some patients retain a disfiguring hypo-pigmentation.
3. Third-degree burn
Diagnosis of third-degree burns is easier than second-degree burn. The scald third-degree wound is pale with no blood supply and almost no exudate. The pain sensation is lost or reduced. Flame burns wound has a carbonized epidermis which can be adherent to the dermis. The wound surface is lower than surrounding normal skin surface, there is a loss of pain sensation, and no exudate appears at the exudation stage. After treated with burn regenerative therapy MEBT/MEBO, sparse exudate can be seen. After the exudation stage, the necrotic tissue begins to liquefy, but this occurs much slower than that of deep second-degree burns wounds. Liquefaction completes in 15-20 days and granulation tissue appears in the wound. The superficial third-degree burn with thermal injury reaching the subcutaneous layer may heal by skin regeneration. A small area of deep third-degree burn wound (diameter<18cm) with thermal injury reaching the muscle layer may heal without skin grafting but with scar formation. Large deep third-degree burns wound needs skin grafting. Pediatric third-degree burns wound is usually dark and red in color. When conventional surgical burns therapy is applied, it is difficult to estimate burn depth accurately, especially to distinguish deep second-degree and third-degree burns.
4. Pathological basis of “three degree four division method” for diagnosis of burn depth
(1). First-degree burn
Only the epidermal layer is injured without blister. The blood vessels are dilatated and the microcirculation is congested. The injured area is red shortly postburn. This area is sensitive to pain, because the sensory nerve endings are still there and endogenous chemicals such as kinin are released from thermal injured tissues, irritating the nerves. First-degree burns wounds heal without scar formation. When treated with conventional therapy, hyperpigmentation may be caused temporarily, but this typically vanishes in a few months. The skin recovers normally. When treated with MEBO, the skin recovers to normal appearance in about half a month.
(2). Second-degree burns
Thermal injury reaches epidermal and dermal layers. The injured area is moist, with blister formation and epidermis exfoliation. Congestion is obvious. If injury reaches the dermal layer, swelling in the dermis and deep tissues may press the blood capillaries and obstruct the blood flow which causes the wound to look pale. The injured area is very sensitive to pain as is the first-degree burn. Second-degree burns can be classified as superficial second-degree burns or as deep second-degree burns.
• Superficial second-degree burns wounds: Some epidermis extended to papilla, so they are not injured. The basal layer of the epidermis, i.e. regenerative layer, survives. The basal cells can divide and regenerate to cover the wound, thus the wound could be completely epidermidalized.
• Deep second-degree burns wounds: Epidermis is completely destroyed, only parts of the skin appendages survive, i.e. basal cells of follicles and sweat glands which are located in the deep part of the dermis. The wound can also be covered and healed by division and regeneration of these surviving cells in the appendages. When conventional surgical therapy is applied, in most cases the wound results in infection and worsens, ultimately healing with epithelialization. Conversely, when MEBT/MEBO is applied, epidermidalization can occur, the full thickness of skin can be completely recovered. Changes in skin pigmentation may occur to different extent.
• Third-degree burns: Progressive stasis zone necrosis and coagulation necrosis of epidermis occur, dermis and deep layer tissues of dermis are completely destroyed by thermal injury. No blood flow can be found in the necrotic area, the wound is pale. When treated with dry-exposed therapy, a black crust may form and even carbonization may occur. In children, wounds are red and black, because children have more water in the tissue and the skin is thinner. In the third-degree burns area, one can see some blood vessels in a thrombotic state. The lesion is not sensitive to pain, because sensory nerve endings are destroyed. The interface of the basal part of the injured area and normal tissue has reduced pain sensation. Small third-degree burns wounds can be covered by wound edge surviving epithelial cell proliferation and regeneration. But for large third-degree burns wounds, skin grafting or epithelial cell transplantation is required. Recently, it was found that sweat gland epithelia in the subcutaneous fatty layer can regenerate to cover the wounds. Accordingly, third-degree wound injury reaching fatty layer is capable of spontaneous healing.
Burns due to different causes may have different depths, so for diagnosis of burn depth, the doctor needs to clearly establish the cause of burn and understand the varied characteristics. For example, burn wounds with carbonized surface may not necessarily be third-degree burns. A moist scald wound with blisters must be a second-degree scald. An acid burns wound with crust is much shallower than a non-crust alkali burns wound.
When applying MEBT/MEBO, the wounds are exposed to the naked eye’s inspection in the whole course, which provides an advantageous condition for clinical diagnosis.
5. “Three degree six division method”
People usually classify burn depth according to the penetration of anatomical structure. i.e. superficial, partial and full-thickness burns. Burns are also classified into three degrees by numbers: first-degree burns, only superficial cell layer is involved; second-degree burns involves basal layer of the epidermis and superficial layer of the dermis, while third-degree burns involves subcutaneous tissue. According to wound manifestation and healing, deep burns wounds can be divided in an even more detailed manner. Second-degree burns can be divided into three grades: Superficial second-degree burns refers to burn injury reaching the basal layer of epidermis with some of the basal layer is still surviving. Superficial deep second-degree burns refers to burn injury reaching the dermal papillary layer while deep second-degree deep burns refers to burn injury reaching the dermal reticular layer. The theoretical basis is that in superficial second-degree burns wounds, the skin microcirculation has been injured but there is no stasis zone and most of the skin structure is retained. In deep second-degree burns wounds, the stasis zone occurs in the dermal papillary layer but epidermal structure is lost while most of the skin appendages are still retained. In deep second-degree deep burns wounds, a microcirculation stasis zone is formed in the dermal reticular layer and only a small part of the appendages is retained.
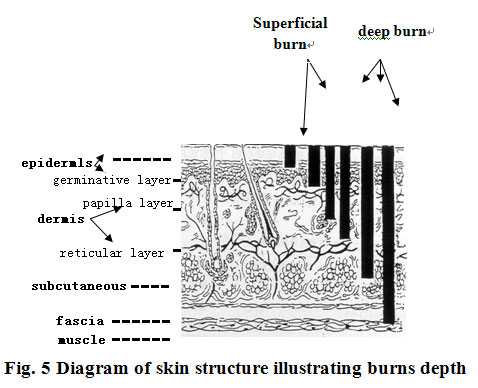
Third-degree burns can be divided into two grades. Superficial third-degree burns refers to necrosis of the dermis, but subcutaneous tissues still have vitality and a small part of the epithelial tissue of the sweat glands in deep subcutaneous areas survives. Deep third-degree burn refers to muscular layer thermal injury. Bone burns refers to bone injury (Fig.5)
In clinical practice, people often find that some burns wounds contain an obvious granulation while, around the lesion, there are a few scattered skin island tissues. This is called mixed-degree burn.